Every March, people around the world come together to bring awareness to endometriosis. So here’s everything you need to know about endometriosis. The painful condition which is estimated to impact around 10% of women and girls globally (around 190 million women and girls of reproductive age) is an inflammatory condition where endometrial tissue grows outside of the uterus.
Endometriosis: Symptoms, Diagnosis, Treatment
What is endometriosis?
Endometriosis is a painful condition and it is estimated that it impacts one out of ten women. It is an inflammatory condition where endometrial tissue (tissue similar to that of the lining of the uterus) is found outside of the uterus. It can be found most often around the ovaries, fallopian tubes, digestive system, bladder and in rare cases up to the chest cavity. This endometrial tissue reacts very much the same way to your menstrual cycle as the tissue lining your uterus and can cause internal bleeding during your period with no way to escape which then causes inflammation, scar tissue and cysts.

What causes endometriosis?
The causes of endometriosis are still not known which is no big surprise when taking into account the fact that this condition is still severely under researched and under diagnosed. Everything you need to know about endometriosis causes:
- Retrograde menstruation (this is when menstrual blood and endometrial tissue flows back into fallopian tubes and abdomen)
- Genetics (this does not explain the cause of it per say but some research indicates you’re at a higher risk for endometriosis if other women in your family also have it)
- Blood or lymph system transport: endometrial tissues are transported to other areas of the body through the blood or lymphatic systems)
Some causes currently being researched:
- Hormonal imbalance: we know that endometriosis and excess oestrogen go hand in hand but causality is yet to be determined. It could be that hormonal imbalance plays a big role with endometriosis.
- Blood sugar regulation issues and elevated cortisol
- Immune system disfunction (women with endometriosis are often found to have compromised immune systems)

Symptoms of endometriosis
Endometriosis causes a wide range of symptoms which vary in intensity from one person to another. The most common symptoms of endometriosis are:
- Dysmenorrhea aka period pains: for women suffering from endometriosis, it goes beyond the cramps that most women experience. Pain killers are unlikely to make a massive difference in pain levels and it can be so debilitating that women suffering from endometriosis are unable to carry on any of their usual day to day activities during their periods.
- Fatigue: the constant elevated inflammation and pain caused by endometriosis can cause real physical and mental fatigue.
- Proctalgia fugax: this pain is described as a very sharp and sudden pain in your rectum. Some women who experience it describe it as a sharp stabbing pain that can come on very suddenly and make you literally jump up from your seat holding on for dear life. This tends to occur particularly during periods and bowel movements. Although women can experience proctalgia fugax without experiencing endometriosis, it can be an indicator of the condition, particularly rectovaginal endometriosis.
- Painful sex: the elevated inflammation and scar tissue associated with endometriosis can make sexual intercourse uncomfortable or down right painful.
- Painful urination.
- Difficulty in fulfilling work and social commitments.
- Fertility issues: the formation of scar tissue and hormonal imbalance associated with endometriosis can lead to an inability to conceive (the prevalence of endometriosis in women with infertility be as high as to 30–50%1).
- Depression: living in constant pain and having to cut back on a social life due to symptoms of endometriosis can feel very isolating and lead to depression.
What is endo belly?
Endo belly is an extremely bloated abdomen and can be a sign of endometriosis. In fact, one study found that 96 percent of women with endometriosis experienced belly bloating compared with 64 percent of women who didn’t have the condition. Your abdomen may be very distended, painful and hard to the touch and it may also be accompanied by nausea, gas pain, constipation and diarrhoea.
Can men can endometriosis?
Endometriosis in men is very unlikely and there have only been about 20 reported cases. The majority of male endometriosis cases are thought to be a consequence of prolonged hormone therapy and abnormally high oestrogen levels.
Diagnosis for endometriosis
Diagnosis is crucial when it comes to everything you need to know about endometriosis. It can take women on average about 8 years to get diagnosed with endometriosis2. This lengthy journey to diagnosis means many women go on to suffer both physically and mentally for close to a decade before finding out their condition and seeking appropriate treatment. There are numerous reasons for this delay to diagnosis:
- The symptoms of endometriosis can sometimes be confused for other conditions
- Severe period pain is often dismissed by medical professionals as something women of reproductive age just have to deal with and women’s pain is notoriously not taken seriously no matter the condition (this gender health gap also means women are 50% more likely to be misdiagnosed when suffering from a heart attack compared to men for example).
- Delays getting seen by GP surgeries and specialists in the UK mean women are more likely to delay seeking medical help
The only way to diagnose endometriosis 100% is through a laparoscopy:
“It’s a procedure done under general anaesthesia which is usually done as a day case. A little camera (the laparoscope) goes through an incision made in the belly button area, which gives an opportunity to see inside the abdomen and the pelvis, making it possible to see the obvious signs of endometriosis forming. That also gives the ability to remove the disease with the aid of the laparoscope at the same time of making the diagnoses. A laparoscopy doesn’t mean that the endometriosis will be completely removed. It should be considered as a chronic condition, and all treatments we put in place are to manage symptoms but won’t always eradicate it. Even with surgical removal, there is a possibility that the condition will come back over the course of a few years. Whilst women are still producing cyclical hormones and having periods, endometriosis can continue / reoccur. Our role is to help manage the symptoms and any fertility problems that crop up as a result.”
Dr Chris Guyer, Consultant at TFP Fertility UK one of the UK’s leading IVF and fertility specialists
For more information on laparoscopy surgery, you can click here.

Endometriosis Treatment
When it comes to treatment for endometriosis, this can vary from one individual to another as it can depend on the severity and localisation of the endometriosis:
“Women should seek medical advice as each case is different. However, to give some background, there are usually three lines to treatment which includes pain management (given that pain is the main symptom) which comes in various guises, so this is often one of the first things we treat. That may be exploring anti-inflammatory medicines combined with a pain relief. Outside of that there are hormonal treatments – commonly that could be the contraceptive pill, so a combined pill with oestrogen and progesterone or progesterone on its own. Both of those preparations are designed to try and suppress some of the hormonal drive to Endometriosis and reduce the inflammatory response that you get from it. There are other hormonal treatments but usually those would be under the guidance of specialists where you are suppressing the ovaries much more than you normally would do with the standard hormone treatments. The other side of it is surgery to try and remove the endometriosis, which is usually done with a procedure called a laparoscopy.”
Dr Chris Guyer, Consultant at TFP Fertility UK one of the UK’s leading IVF and fertility specialists
When it comes to symptom management, there are a few healthy lifestyle habits that you can adopt:
- Diet: a balanced and healthy diet is crucial when it comes to managing symptoms. Try avoiding trans fat, processed foods, high consumption of red meat, alcohol3 and gluten4. Instead, focus on nutrient dense food and appropriate intakes of fiber.
- Getting enough sleep: it’s a fact that women on average need more sleep than men (at the very least 7 hours a night but some individuals ideally need up to 9 hours). Getting quality sleep has been proven to help hormonal balance and hormonal balance has been shown to impact sleep quality so this is a vicious circle for many (READ MORE: Women’s Sleep Tips: How To Fall Asleep Faster And Sleep Better).
- Exercise: regular low impact exercise such a walking or swimming is crucial to health and can help hormonal imbalance (the very act of exercise can help with excess oestrogen). This is easier said than done for women going through endometriosis as the pain and fatigue can prevent them from exercising so instead of going for high intensity exercise which will raise cortisol levels, try walking for 30 minutes to 1 hour per day (ideally more if you can). A foldable walking treadmill at home is a great option as it allows you to easily stop if you’re feeling unwell and can be used whilst working, watching TV or ironing for example (we love this walking treadmill from Amazon).
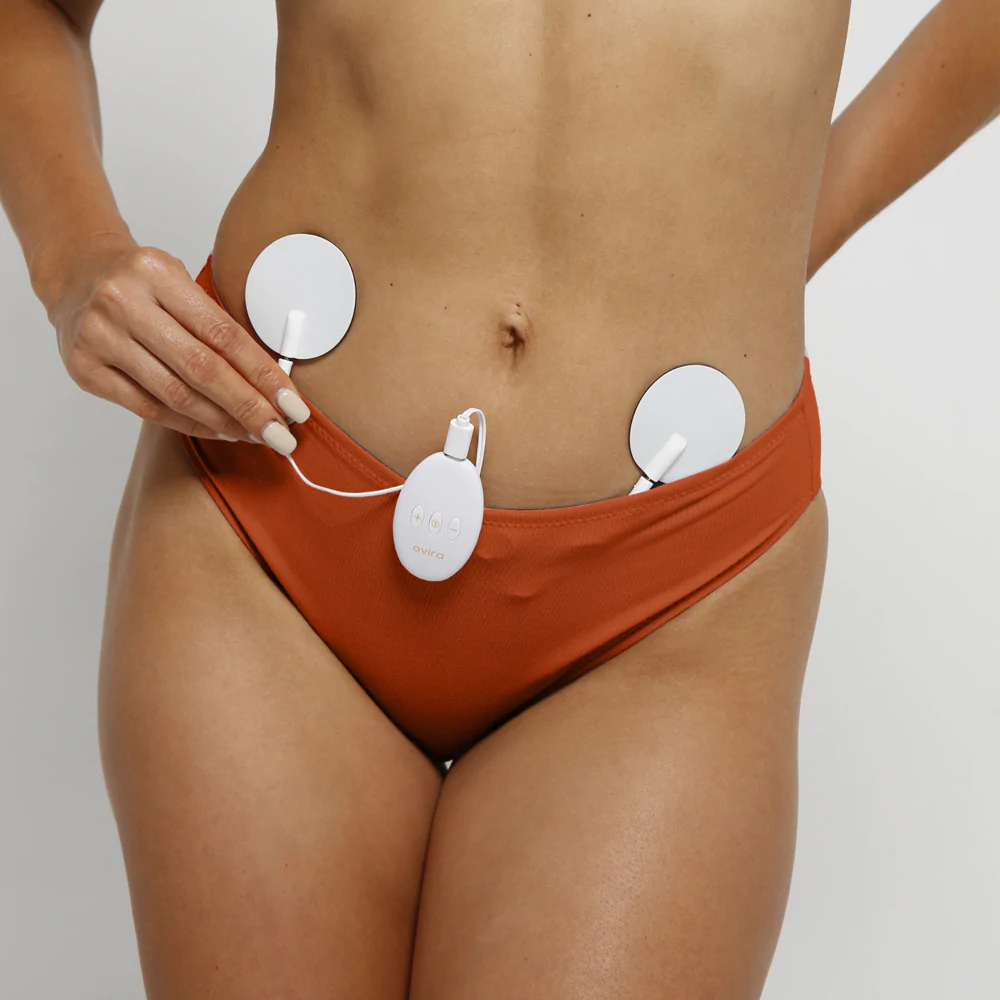
Lastly when it comes to pain management, some women have reported great success with TENS devices (transcutaneous electrical nerve stimulation). These little electrical devices are connected to gel pads which are then applied to the abdomen or back and send mild electrical current which reduce the pain signals going to the spinal cord and brain. They also stimulate the production of endorphins, which are the body’s natural painkillers.

Best supplements for endometriosis
Last but not least when discussing treatment and everything you need to know about endometriosis. Although supplements alone are not a cure for endometriosis, some studies have shown beneficial use of certain supplements in symptom management:
- One small study involved 59 women with endometriosis. These women supplemented with 1,200 international units (IU) of vitamin E and 1,000 IU of vitamin C which showed a reduction in chronic pelvic pain and a decrease in inflammation5.
- One study found that consumption of curcumin/turmeric inhibited the endometrial cells by reducing estradiol production6.
- Some brands such as Wild Nutrition also offer supplement blends to help support hormonal balance
Endometriosis awareness in the workplace
Endometriosis UK have created a very useful scheme called Endometriosis Friendly Employer which allows employer to confirm their commitment to developing a work environment and culture that enable employees with endometriosis to thrive at work:
“Through the scheme, Endometriosis UK provides guidance for employers on how to support employees with endometriosis and menstrual health conditions, and work towards improving the work environment in three key areas:
1. Leadership and management support
2. Tackling stigma and changing culture
3. Communications
From our work with those with the disease and employers, we believe that by overcoming the challenges individuals may face in the workplace due to lack of knowledge or misunderstanding of endometriosis and other menstrual health conditions, Endometriosis Friendly Employers will see improvements in employee wellbeing, productivity and performance, employee engagement and morale.”
Endometriosis UK
If you believe you have been or are being treated unfairly by your employer as a result of your endometriosis condition, you can reach out to Citizen Advice Bureau for free help and advice:
Adviceline (England): 0800 144 8848
Advicelink (Wales): 0800 702 2020
Adenomyosis vs endometriosis?
When discussing everything you need to know about endometriosis it’s important to discuss similar conditions. The main difference between adenomyosis vs endometriosis is where the endometrial tissue grows. In certain cases, you can suffer from both adenomyosis and endometriosis.
Adenomyiosis is a condition that cause endometrial tissue to bury into the muscular wall of the womb. This can cause similar symptoms to endometriosis such as heavy and painful periods, bloating, painful intercourse and infertility.

Celebrities with endometriosis
More and more celebrities and public figures have been speaking out about their diagnosis with endometriosis and how this has impacted their lives:
- Leah Williamson: the England captain has revealed that a flare-up of her endometriosis symptoms almost meant she couldn’t compete in England’s victorious 2022 European Championship campaign.
- Hilary Mantel: the novelist revealed her lifelong struggle with endometriosis. She opened up about her struggle to get a diagnosis, getting taken seriously by doctors who at one point offered her psychiatric treatment. Sadly Hilary Mantel passed away in September 2022.
- Bindy Irwin: the daughter of the late conservationist and adventurer Steve Irwin has recently revealed in an emotional Twitter post that she has battled with endometriosis for the last ten years. Talking about her journey to a diagnosis Bindy said: “a doctor told me it was simply something you deal with as a woman and I gave up entirely, trying to function through the pain.”
- Susan Sarandon: the actress has been vocal about her struggle with endometriosis and talking about doctors dismissing sufferers she even said at the Endometriosis Foundation in 2016: “This isn’t part of being a woman […] Something can be done.”
- Cyndi Lauper: the singer opened about having endometriosis in her 30s. She struggled with infertility and finally gave birth to her son Declyn at age 44.
- Emma Bunton: the singer and member of the Spice Girls struggled with endometriosis and was diagnosed at the age of 25.
Below The Belt endometriosis documentary
Below The Belt is a new documentary addressing endometriosis, the difficult road to a diagnosis and the widespread issues with the American healthcare system.
“Through the lens of endometriosis, a disease that affects 1 in 9 women, the film shows how women are often dismissed, discounted & disbelieved. From societal taboos and gender bias to misinformed doctors and profit-driven healthcare, the film reveals how millions are silenced and how, by fighting back, we can improve healthcare for everyone.”
“We deserve to be believed. We deserve to be understood. We deserve to be empowered to understand ourselves, our bodies and any medical treatments presented to us. We deserve better across the entire healthcare system. Below the Belt aims to revolutionise the status quo so that people with endometriosis get what we deserve – the right to live healthy, informed, fulfilling lives.”
Executive Producer Rosario Dawson
We do not have a screening date in the U.K. as of yet however stay tuned to find out information on its release.
Endometriosis helpline:
Last but not least for everything you need to know about endometriosis is how to get help and advice.
Endometriosis U.K. offers a helpline for anyone who is or thinks they might be struggling with endometriosis: 0808 808 2227
Please be aware that their helpline team are unable to provide medical advice and can only talk about endometriosis based on their own experience.
For any medical advice, you can also reach out the NHS helpline by dialling 111.
Sources Everything You Need To Know About Endometriosis:
1 Meuleman C, Vandenabeele B, Fieuws S, Spiessens C, Timmerman D, D’Hooghe T. High prevalence of endometriosis in infertile women with normal ovulation and normospermic partners. Fertil Steril 2009;92(1):68-74.
2 Endometriosis in the UK: Time for Change – APPG on Endometriosis Inquiry Report 2020
3 Marziali M, Venza M, Lazzaro S, et al. Gluten-free diet: a new strategy for management of painful endometriosis related symptoms? Minerva Chirurgica. 2012 Dec;67(6):499-504. PMID: 23334113.
4 Joanna Jurkiewicz-Przondziono, Magdalena Lemm, Anna Kwiatkowska-Pamuła, Ewa Ziółko, Mariusz K. Wójtowicz, Influence Of Diet And The Risk Of Developing Endometriosis, 2017.
5 Santanam N, et al. (2013). Antioxidant supplementation reduces endometriosis-related pelvic pain in humans.
6 Zhang Y, Cao H, Yu Z, Peng HY, Zhang CJ. Curcumin inhibits endometriosis endometrial cells by reducing estradiol production. Iran J Reprod Med. 2013 May;11(5):415-22. PMID: 24639774; PMCID: PMC3941414.





